By Dr Emily Amos | Mindfulness, Lifestyle Medicine and Stress Management | Director, Whole Hearted Medicine
If you are reading this, there is a reasonable chance you are one of a relatively small group of people who has decided, often at some personal and professional cost, that the way medicine treats its own people is not good enough.
You have probably sat in a meeting where burnout was acknowledged in one breath and normalised in the next. You have likely watched colleagues quietly disintegrate under workloads that would be considered unacceptable in almost any other profession, while the institutional response amounted to little more than a mindfulness leaflet and a reminder about the Employee Assistance Programme. You may have tried to raise the issue formally and found yourself navigating a culture that is, at best, politely resistant and, at worst, actively hostile to the conversation.
You are not imagining it, and you are not alone.
But I also want to say this clearly: what you are doing matters enormously, even when it doesn’t feel like it. Especially when it doesn’t feel like it.
Because what you are doing, whether you use this language or not, is attempting to diffuse an innovation through one of the most change-resistant professional cultures in existence. So, understanding the science of how that process actually works may be one of the most practically useful things available to you right now.
The Moment That Changed the Conversation
Before we get into the framework, we need to acknowledge the context. Because doctor wellbeing did not exist in a vacuum before 2020, but COVID-19 did something that years of advocacy had struggled to achieve: it made it impossible to look away.
The pandemic placed doctors and healthcare workers on the front line of a global crisis with inadequate protective equipment, shifting protocols, impossible decisions, and grief on a scale that most had never encountered in their professional lives. The moral injury was profound. The psychological toll was documented, publicly, in real time. Doctors spoke openly about their mental health in ways the profession had historically discouraged. Some did not survive.
The public, for perhaps the first time, glimpsed what medicine had been quietly absorbing for decades.
COVID did not create the doctor wellbeing crisis. It revealed it. The research had been building for years. Tait Shanafelt and colleagues at Stanford had already established, through a series of large-scale national surveys, that burnout among US physicians was not only prevalent but worsening, rising from 45.5% of physicians reporting at least one symptom in 2011 to significantly higher rates across subsequent years.¹ During the acute phase of the pandemic, that figure climbed to 62.8%, a level that made the pre-existing crisis impossible to attribute to individual frailty or lack of resilience.² Alongside burnout, the data on physician suicide had long painted a sobering picture: a systematic review and meta-analysis of 25 studies found that the overall standardised mortality ratio for physician suicide was 1.44 compared with the general population, with female physicians at nearly twice the risk of their male counterparts.³
These were not pandemic phenomena. They were pre-existing conditions that a global emergency finally made visible enough to demand a response.
That visibility matters for those of us working on culture change, because it created something that the Diffusion of Innovation Theory tells us is absolutely essential for an idea to move through a population. It created a critical mass of people who could no longer reasonably deny that there was a problem worth solving.
What Is the Diffusion of Innovation Theory, and Why Does It Matter Here?
In 1962, communication scholar Everett Rogers published Diffusion of Innovations, asking a question that turns out to be deeply relevant to anyone trying to change medical culture: why do some ideas spread, and others stall?
Rogers found that when any new idea, behaviour, or practice enters a population, it doesn’t land evenly. It moves through five distinct groups, each with its own relationship to change, its own motivations, and its own specific needs before adoption becomes possible. The speed at which something spreads depends not on the quality of the idea alone, but on how well it is understood, communicated, and supported at each stage of that journey.
Doctor wellbeing as a genuine clinical and institutional priority is, by any reasonable measure, still in the early stages of that journey within medicine. It has passionate advocates. It has a growing evidence base. It has the tailwind of a post-pandemic cultural shift that has made mental health discussion more acceptable across society. But it has not yet reached what Rogers would call critical mass within the medical profession itself, and understanding why requires us to look honestly at each of the five groups and what they need.
The Five Adopter Groups Within Medicine
1. Innovators (approximately 2.5% of the medical workforce)
You probably know these people. They may, in fact, be you.
These are the clinicians, educators, and healthcare leaders who were talking about physician burnout, moral injury, and systemic cultural dysfunction in medicine long before it was a safe or particularly popular thing to do. They were writing about it in journals, raising it in meetings, building programmes with limited resources and even more limited institutional support, and absorbing the professional scepticism that often greets those who name uncomfortable truths in hierarchical organisations.
One of the most important early contributions from this group came from Shanafelt and Noseworthy, whose landmark 2017 paper in Mayo Clinic Proceedings argued that physician burnout is fundamentally a system issue, not an individual one, and that approximately 80% of the burnout challenge is driven by characteristics of the work environment, organisational culture, and professional culture rather than by deficits in individual resilience.⁴ That reframe, from personal failing to structural problem, is the intellectual foundation on which the entire doctor wellbeing movement now rests. It took innovators to put it into the literature. It is now the lens through which the rest of the conversation must be had.
Innovators in this space are intellectually driven, systems-oriented, and comfortable operating on the fringe of accepted discourse. They don’t need consensus before they act. They need evidence, a problem worth solving, and enough personal conviction to keep moving when the culture pushes back.
If this is you, your role in this movement is irreplaceable. You are the reason the conversation exists at all. But it is also worth naming something that innovators in any field sometimes struggle with: the skills that make you exceptional at identifying and championing a new idea are not always the same skills required to bring a sceptical majority along with you. That is not a failing. It is simply a different part of the work, and it may require different tools and different allies.
What innovators in medicine need: connection with other innovators to avoid isolation, access to robust research to support the evidence base, and strategic support in translating visionary advocacy into institutional change.
2. Early Adopters (approximately 13.5% of the medical workforce)
Early adopters are the most important group for anyone trying to shift medical culture, and it is worth spending time here.
These are the clinicians, and perhaps even department heads, medical educators, or healthcare executives; who are not yet publicly championing doctor wellbeing, but who are privately persuaded that something needs to change. They have watched colleagues burn out. They have their own quiet history with the cost of the culture. They are observing what the innovators are doing, and they are paying attention.
What distinguishes early adopters from innovators is that they move with more deliberation. They need to see credible evidence before they act, and they need to feel that acting will not significantly damage their professional standing. In a culture as reputation-conscious as medicine, that second condition is not trivial. But once early adopters are genuinely convinced, they carry enormous weight. These are the opinion leaders. The people that medical institutions actually listen to.
The role of early adopters in spreading doctor wellbeing as a cultural priority cannot be overstated. When a respected clinician speaks openly about their experience of burnout, it does more for cultural change than a hundred advocacy leaflets. When a clinical director integrates protected wellbeing time into a department’s structure, colleagues in other departments notice. When a medical school dean makes student and faculty wellbeing a visible institutional priority, it signals to the entire organisation that this is now a legitimate concern.
COVID accelerated the movement of a number of people from this group into more active positions. The pandemic gave early adopters in medicine the social permission and the undeniable evidence they needed to step forward.
At Whole Hearted Medicine, we see this group clearly and consistently. Over six years and nearly 30 retreats, the majority of the more than 400 doctors who have come to us from across Australia and New Zealand have been early adopters. These are clinicians who arrived already persuaded that something needed to change, both within themselves and within their profession. What they were looking for was not more information. It was connection, community, and a structured space to translate their conviction into something they could carry back into their working lives. Many of them have done exactly that, taking their energy, their insight, and their renewed sense of purpose back into hospitals, practices, and medical schools, and creating what I can only describe as ripples of change. That is the early adopter doing what Rogers always said they do best: building the bridge between the fringe and the majority.
What early adopters in medicine need: high-quality, peer-reviewed evidence they can cite with confidence, institutional frameworks they can adopt without reinventing from scratch, and the visible support of credible professional bodies. They need to know that moving on this will not cost them more than it gains.
3. Early Majority (approximately 34% of the medical workforce)
This is the group that will determine whether doctor wellbeing becomes genuinely embedded in medical culture or remains a peripheral conversation among committed advocates.
The early majority in medicine are the clinicians and healthcare professionals who are aware of the wellbeing agenda, probably sympathetic to it in principle, but not yet doing anything meaningfully different as a result. They are watching. They are weighing, and they are looking for social proof that change is both possible & professionally safe.
This group responds to lived experience above abstract argument. A colleague who has completed a structured wellbeing programme and returned to work visibly different. A ward culture that has genuinely shifted and whose outcomes, both clinical and human, have improved as a result. A medical school cohort that has been through a curriculum redesigned with wellbeing at its core, and who are entering the profession in better shape than their predecessors.
The early majority are not waiting for someone to convince them intellectually. They are waiting for enough people around them to make the change that it starts to feel normal rather than exceptional. They are waiting for the culture to shift just enough that following it carries less risk than it currently does.
Something I find genuinely encouraging, and that I think represents a meaningful shift in the landscape, is that at our Whole Hearted Medicine retreats, we are now seeing a growing number of doctors who sit squarely in this early majority. These are clinicians who, a few years ago, might not have considered attending. What has brought them is exactly what Rogers’ model would predict: they have watched someone they respect, a colleague, a registrar, a friend from training, come back from one of our retreats changed in some visible and credible way. The social proof is beginning to accumulate. The tipping point, while not yet reached, feels closer than it did.
What the early majority in medicine need: visible, credible case studies from within their own professional world. Peer testimony carries more weight than external advocacy here. Practical, low-barrier entry points into wellbeing practices and cultural change. Evidence that the cost of engagement, in time, energy, and professional capital, is manageable.
4. Late Majority (approximately 34% of the medical workforce)
The late majority in medicine are sceptical, and in many cases, they have earned their scepticism.
These are the clinicians and leaders who have watched wellness initiatives come and go. They have seen the yoga class added to the staff intranet, the resilience workshop offered as a response to a 70-hour working week, the wellbeing survey administered during the most pressured period of the year. They have experienced wellness as a performance, a box-ticking exercise, a way of managing the optics of a broken system without addressing its structural failures.
Their resistance is not irrational. It is, in many cases, the appropriate response to years of being offered the wrong solution to the right problem. The research is clear that individual-level interventions alone are insufficient to address what is, at its core, a systemic issue. As Shanafelt and Noseworthy articulated so precisely, burnout cannot be solved by asking individuals to be more resilient within structures that remain unchanged.⁴
What will reach the late majority is not more advocacy. It is structural, visible, undeniable change. Reduced working hours. Protected time for clinical supervision and peer support. Genuine psychological safety in reporting errors and expressing distress. A hiring and promotion culture that values whole physicians rather than simply productive ones. When the late majority see that the institution itself has changed, not just its language, they will begin to move.
What the late majority in medicine need: systemic change they can observe and verify. Institutional commitment that is demonstrated through policy and resource allocation, not just communication. They need to see that this time, it is different. That is a high bar. It is, however, the correct bar.
5. Laggards (approximately 16% of the medical workforce)
It is tempting, in a piece written for changemakers, to spend little time on this group. But I think that would be a mistake.
Laggards in the context of medical culture change are not simply obstructive. Many are doctors who have survived a demanding career by building a particular internal architecture around endurance, self-sufficiency, and the suppression of emotional and physical need. That architecture did not emerge from weakness. It emerged from a training culture that rewarded it, and in some cases required it for survival.
When you ask someone who has built their professional identity on not needing support to embrace a culture of wellbeing and psychological openness, you are not asking them to adopt a new habit. You are, in some ways, asking them to revise a core part of how they understand themselves as a doctor. That is not a small thing.
Laggards in this space also often hold seniority. They have institutional power, and their visible resistance, whether through active opposition or simply the modelling of the old culture, carries significant weight in departments and schools where hierarchy matters.
The approach that works here is not confrontation. It is patient, respectful engagement that does not require explicit conversion. Sometimes the goal is simply to reduce active opposition and create space for the culture around them to shift. Sometimes, with time and the right relationships, more than that becomes possible.
What laggards in medicine need: to have their professional experience honoured, not dismissed. Engagement that does not threaten their identity or their legacy. Small, unthreatening exposures to a different way of thinking about medical culture, and the understanding, from those of us doing this work, that their resistance is part of the system we are trying to change, not simply a personal obstacle.
What This Means for Those Leading the Change
If you are a changemaker in medicine, this framework asks something of you that goes beyond passion and conviction. It asks you to be strategic about where you invest your energy, who you are speaking to at any given moment, and what that person actually needs from you to move.
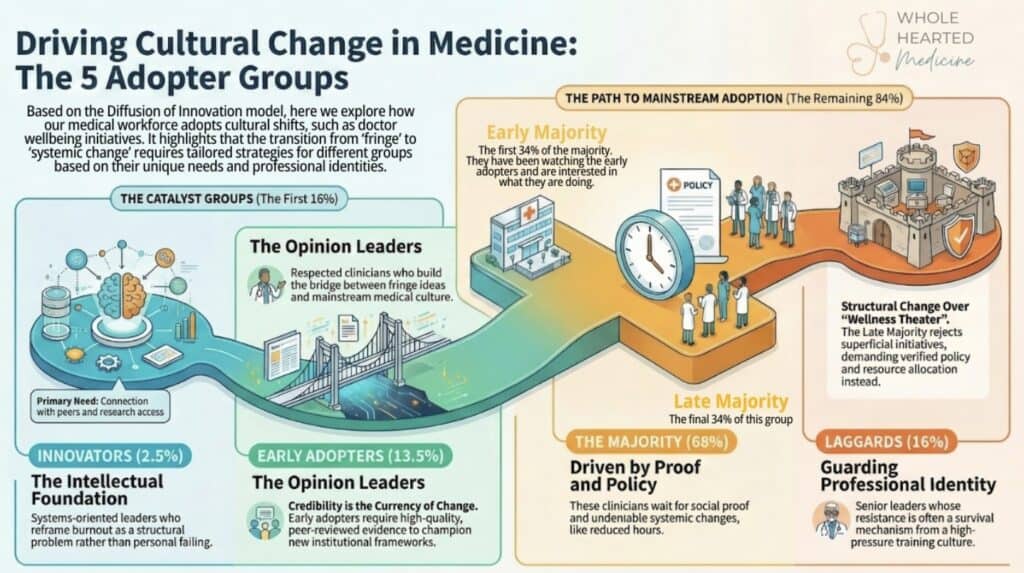
It asks you to recognise that the innovators need community and protection from the isolation that comes with being ahead of the curve. That the early adopters need credible evidence and institutional permission. That the early majority need to see the change working in real people’s lives before they will risk joining it. That the late majority need structural proof, not persuasion, and that laggards need patient respect, not conversion.
Over the past six years, I have watched something quite specific happen. Doctors arrive carrying the weight of a culture that has taken a great deal from them. They invest in connection, in learning, and in growth- and they leave with something that is genuinely difficult to manufacture any other way: a sense of hope that is grounded in community rather than in isolation.
That hope travels back into workplaces. It shows up in conversations that wouldn’t otherwise have happened, in small structural changes that someone finally felt equipped to advocate for, in a registrar who saw their supervisor model vulnerability and filed it away as permission to do the same. These are the ripples. They are real, and they accumulate.
More recently, through our Whole Hearted Leadership retreats delivered in collaboration with Capstan Partners, we have extended this work specifically to medical leaders, equipping them with coaching skills and leadership frameworks that allow them to take their commitment to doctor wellbeing and amplify it within their sphere of institutional influence. This is, in Rogers’ terms, a direct investment in the early adopter and early majority interface. It is how we accelerate the spread. Not by pushing harder, but by equipping the right people with the right tools to lead from where they already stand.
It is also, I’ll be honest, one of the most hopeful things I have been part of in my professional life.
Because the theory tells us that every group eventually moves. The innovators and early adopters are already in motion. The early majority are watching closely and, increasingly, stepping forward. The late majority will follow when the culture shifts enough to carry them. Even the laggards, when given enough time and the right conditions, adapt.
You are not pushing against something immovable. You are pushing against something that moves slowly, and that is a very different thing.
Keep going.
Dr Emily Amos is a specialist in mindfulness, meditation, lifestyle medicine and stress management, and the Director of Whole Hearted Medicine. She works with clinicians, healthcare organisations, and medical educators across Australia and New Zealand to build evidence-informed, sustainable approaches to practitioner wellbeing.
👉 Learn about Whole Hearted Medicine
References
- Shanafelt TD, Boone S, Tan L, et al. Burnout and satisfaction with work-life balance among US physicians relative to the general US population. Arch Intern Med. 2012;172(18):1377-1385. doi:10.1001/archinternmed.2012.3199
- Shanafelt TD, West CP, Dyrbye LN, et al. Changes in burnout and satisfaction with work-life integration in physicians during the first 2 years of the COVID-19 pandemic. Mayo Clin Proc. 2022;97(12):2248-2258. doi:10.1016/j.mayocp.2022.09.002
- Dutheil F, Aubert C, Pereira B, et al. Suicide among physicians and health-care workers: a systematic review and meta-analysis. PLoS ONE. 2019;14(12):e0226361. doi:10.1371/journal.pone.0226361
- Shanafelt TD, Noseworthy JH. Executive leadership and physician well-being: nine organisational strategies to promote engagement and reduce burnout. Mayo Clin Proc. 2017;92(1):129-146. doi:10.1016/j.mayocp.2016.10.004


